Did you know that over 50 million Americans suffer from sleep disorders? If you’re one of them, understanding how a sleep study is performed can be your first step toward better rest. A sleep study, often referred to as polysomnography, allows healthcare professionals to monitor your sleep patterns and identify issues such as sleep apnea or insomnia. In this guide, we’ll walk you through the entire process step-by-step-from what to expect during your consultation to the setup of equipment in a sleep lab or at home. Whether you’re feeling unsure or anxious about the procedure, we aim to provide you with clear insights, ensuring you feel empowered and informed as you embark on your journey to better sleep. Read on to uncover the details that can help you achieve the restful nights you deserve.
How Sleep Studies Work: Understanding the Basics
Understanding how sleep studies work is crucial for anyone struggling with sleep issues. A sleep study, also known as polysomnography, is a comprehensive test used to diagnose sleep disorders. During this process, a variety of bodily functions are monitored while you sleep, helping healthcare providers understand your sleep patterns and any disturbances that might be occurring.
Before the study begins, your physician will likely recommend keeping a sleep diary for a week or two. This helps track your sleep habits, patterns, and any symptoms you may be experiencing. This information can be invaluable in guiding the type of sleep study that might be necessary. On the night of the study, you’ll arrive at a sleep center or perform an at-home test, depending on what your healthcare provider recommends.
The sleep study itself typically involves sensors placed on your body to measure brain waves, oxygen levels, heart rate, and breathing patterns. In a lab setting, skilled technicians will monitor these parameters throughout the night. If you’re conducting an at-home study, you will receive a device that is easy to set up yourself, usually requiring only a few simple steps.
What sets sleep studies apart is their thoroughness. Not only do they provide insight into sleep stages (such as REM and non-REM sleep), but they also uncover potential issues like sleep apnea, restless leg syndrome, or other conditions. After the study, the recorded data is analyzed, and a report is generated which will help your doctor develop a tailored treatment plan. Each of these stages is crucial in accurately diagnosing sleep-related health issues, thereby empowering you to take informed steps towards better sleep health.
What Happens Before Your Sleep Study
Before embarking on a sleep study, it’s crucial to understand the steps leading up to it, as these preparations can vastly influence the outcome and your comfort throughout the process. One of the first things your healthcare provider may suggest is maintaining a sleep diary. Over one to two weeks, record your sleep patterns, including when you go to bed, wake up, how often you wake during the night, and any symptoms you experience-like daytime sleepiness or snoring. This proactive measure helps your healthcare team tailor the sleep study to meet your specific needs.
As the study date approaches, make sure to discuss with your doctor any medications you’re currently taking. Some substances, such as sleep aids, stimulants, or even caffeine, can impact sleep quality and may need to be adjusted before the test. A good rule of thumb is to follow any specific instructions provided to you, which are designed to yield the most accurate results.
On the evening of the sleep study, you’ll either head to a specialized sleep center or prepare for an at-home testing procedure, depending on the recommendation of your healthcare professional. If you’re visiting a sleep lab, it’s often a comfortable environment designed to mimic normal sleeping conditions, so you may want to bring along familiar items from home, like your pillow or blanket, to help ease any anxiety. Similarly, for at-home studies, the equipment provided is usually straightforward and user-friendly, often involving just a few steps for setup, such as placing sensors on your body.
Expect to be briefed thoroughly by the sleep technician or your healthcare provider about what to anticipate that night. Understanding the setup, including how sensors will monitor various bodily functions-like brain waves, heart rate, and oxygen levels-can demystify the process. Knowing what will happen before you arrive helps reduce anxiety and set the stage for a smoother experience, ultimately ensuring your sleep study is as informative and effective as possible.
Step-by-Step: The Sleep Study Process
When preparing for a sleep study, understanding the specific steps involved can alleviate apprehensions and empower you as an informed participant. The sleep study process typically begins well before the actual night of testing, focusing on thorough preparation and understanding of what will happen.
Initially, you’ll meet with a sleep specialist who will review your sleep history and discuss your current symptoms. This consultation is vital, as it allows the practitioner to determine the best type of sleep study for you. Here’s what you can generally expect:
1. Pre-Study Consultation
During your initial appointments, your healthcare provider will assess your medical history and any sleep-related complaints. This may involve questions about your sleep patterns, daily routines, and possible medications impacting your sleep. Be honest about your experiences; this information helps tailor the sleep study to your specific needs.
2. Choosing the Type of Study
Based on the consultation, your healthcare provider will recommend the appropriate sleep study. Common options include:
- Polysomnography (PSG): An overnight study in a sleep lab that monitors brain waves, oxygen levels, heart rate, and breathing.
- Home Sleep Apnea Testing (HSAT): A simplified version of PSG performed at home using portable equipment.
3. Preparing for the Study
Before the study, you might keep a sleep diary for a week to document your sleep habits. This practical tool assists your provider in identifying patterns that may affect your sleep quality. Discuss any medications you take, as some may require adjustments leading up to the test.
4. Night of the Study
On the night of the study, whether in a clinic or at home, you’ll set up your equipment if it’s a home test or be guided through the process at the lab. Expect to wear several sensors that monitor physical activities while you sleep-these sensors are generally non-invasive and designed for comfort. A technician will brief you on the setup, which simplifies the procedure.
Understanding each of these steps helps demystify the sleep study process. By knowing what to expect, you can relax and focus on the goal: gaining valuable insights into your sleep health to enhance your overall well-being.
Types of Sleep Studies: Which One is Right for You?
When considering a sleep study, understanding the distinctions between the various types of assessments can significantly impact the path to better sleep health. The choice of study often hinges on your specific symptoms, lifestyle, and the healthcare provider’s recommendation. By familiarizing yourself with common sleep study options, you can make an informed choice that best aligns with your needs.
Polysomnography (PSG)
Polysomnography is the gold standard for diagnosing sleep disorders, performed overnight in a specialized lab. This comprehensive test measures multiple parameters-brain waves, oxygen levels, heart rate, and breathing patterns-allowing for an in-depth analysis of sleep stages. While it may seem intimidating, patients typically find the environment comfortable, and technicians ensure a supportive atmosphere. Ideal for those exhibiting symptoms of severe sleep disorders, such as sleep apnea or narcolepsy, PSG can provide the clearest picture of your sleep health.
Home Sleep Apnea Testing (HSAT)
For those who experience symptoms suggestive of sleep apnea but may not require a full in-lab evaluation, Home Sleep Apnea Testing is a practical solution. This method involves a simplified setup performed in the comfort of your home using portable equipment. While HSAT is generally less comprehensive than PSG, it effectively monitors key indicators such as breathing, oxygen levels, and heart rate. This option is especially useful for individuals reluctant to spend a night in a lab or those with moderate symptoms. However, the trade-off may involve missing other sleep-related issues that a more extensive study could uncover.
Considerations for Your Decision
Choosing the right sleep study isn’t solely about the technical aspects; it’s also about your comfort and convenience. Factors to consider include:
- Severity of Symptoms: Severe symptoms typically warrant a more detailed analysis, such as PSG.
- Comfort with Technology: Some may feel more at ease conducting a test at home using HSAT, while others prefer the thoroughness of a lab setting.
- Insurance Coverage: Check with your provider to understand what studies are covered, as this can influence your choice.
By weighing these factors carefully, you can choose a sleep study type that not only addresses your symptoms but also fits your lifestyle. Remember, the ultimate goal is to discover what might be affecting your sleep and enable you to achieve more restful nights.
Preparing for Your Sleep Study: Tips and Tricks
Before stepping into the world of sleep studies, a little preparation can go a long way in ensuring a smooth and stress-free experience. Knowing what to expect and how to get ready can make a significant difference in how comfortable and confident you feel during the test. Arm yourself with the right tips to set the stage for a restful night of observing your sleep patterns.
Start by discussing your sleep study with your healthcare provider. It’s important to ask any questions you may have regarding the procedure, what to expect, and how to prepare. Understanding the specifics will not only alleviate anxiety but also allow you to pinpoint any particular issues that need to be addressed during the study. If you’re undergoing polysomnography (PSG), take note that you may need to adjust your sleep schedule in the days leading up to the test. Try to maintain a steady sleep routine; this consistency will help provide more accurate results.
Another key aspect of preparation involves your pre-study habits. On the night before your appointment, limit caffeine intake and refrain from alcohol, as both can interfere with your sleep quality. Ensure you have a light dinner and arrive at the sleep center wearing comfortable clothing. If you’re a habitual user of sleep aids, consult your doctor to discuss whether to continue their use before the test. Bringing along any personal items, like your favorite pillow or blanket, can also contribute to creating a more familiar and soothing environment.
By taking these steps, you can enhance the effectiveness of your sleep study, ensuring that the data collected reflects your true sleeping patterns and helps your healthcare provider recommend the most appropriate interventions for your sleep health. Remember, knowledge is power-being well-prepared is the best way to pave the way for better sleep.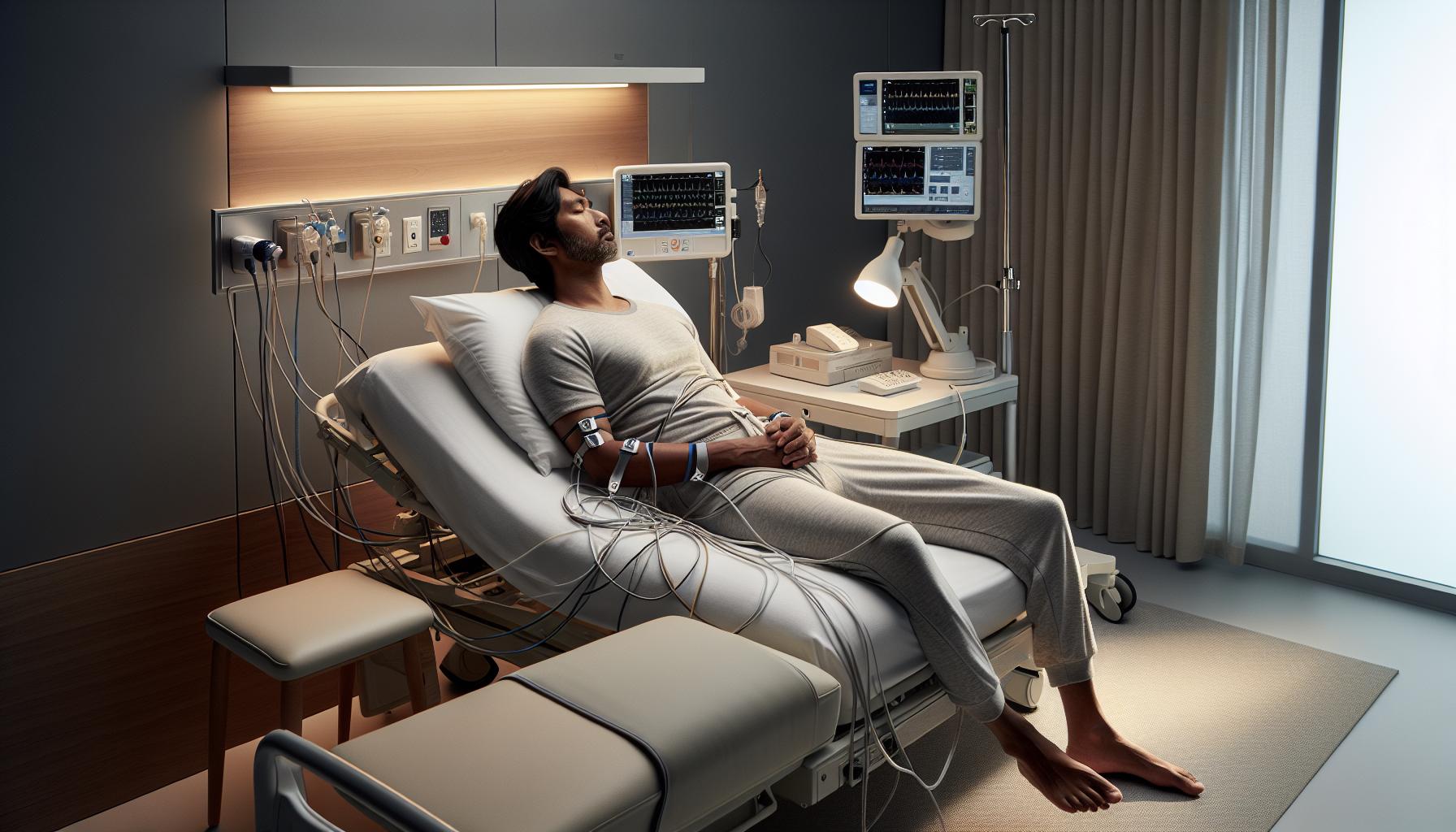
What to Expect During Your Sleep Study Night
As you prepare for your sleep study night, it’s natural to feel a mix of excitement and anxiety. Understanding the flow of the evening can help alleviate some concerns, allowing you to focus on what matters-your sleep health. Typically, you’ll arrive at the sleep center in the early evening. The first step is a brief check-in process where you’ll review your medical history and discuss any specific sleep issues with the sleep technician. This conversation ensures that your needs are fully understood and that the study can be tailored appropriately.
Once settled, you will be guided to your private room, which will resemble a standard bedroom outfitted with monitoring equipment. You’ll be asked to change into comfortable sleepwear. The technician will attach various sensors to your body to monitor your brain waves, heart rate, breathing patterns, and movements throughout the night. While this might feel a bit awkward at first, these sensors are typically lightweight and won’t hinder your ability to sleep comfortably. Expect attachments on your scalp, face, chest, and legs, but rest assured, they’re designed to be non-invasive.
After the setup, you’ll be given time to wind down and prepare for sleep. This might involve some relaxation exercises, reading, or simply lying back in the dim light of the room. The sleep technician will leave the room to allow you to settle in, but they’ll be monitoring you closely through a camera and will remain just outside to assist if necessary. This monitoring ensures you’re comfortable and allows for immediate attention if any issues arise during the night.
Throughout the study, you may wake up at various points, which is perfectly normal. The purpose of the monitoring is to capture your sleep stages and patterns. In the morning, once the study concludes, the technician will gently wake you, disconnect the sensors, and ensure your safe exit. Expect a follow-up appointment to discuss your results, where the data collected will help determine any potential sleep disorders and inform the next steps in your treatment plan. Being prepared and knowing what to expect can transform this experience into a pivotal moment for improving your sleep health.
Interpreting Sleep Study Results: A Simple Guide
Understanding the results of your sleep study is crucial for improving your sleep health. After the sleep technician gathers data on your brain waves, heart rate, and breathing patterns, this information is analyzed by a qualified sleep specialist. They will look for specific indicators to diagnose any sleep disorders you may have. The results can provide insights about sleep architecture, including the time spent in various sleep stages such as REM and deep sleep.
Key Metrics in Sleep Study Results
The sleep report will typically include the following components:
- Apnea-Hypopnea Index (AHI): This metric indicates the severity of sleep apnea by measuring the number of apneas (complete stops of breathing) and hypopneas (partial blockages of airflow) per hour of sleep.
- Oxygen Levels: A drop in oxygen saturation levels during sleep can signal breathing difficulties or disruptions.
- Sleep Stages: Report may detail time spent in different sleep stages, including light sleep, deep sleep, and REM sleep, helping to identify problems in sleep quality.
- Movement and Position: Analysis of movement patterns can highlight issues like insomnia or discomfort leading to awakenings.
Getting your results interpreted can feel overwhelming, but don’t hesitate to ask your doctor to explain each element and how it relates to your sleep health. Having a clear understanding empowers you to actively participate in your treatment plan, whether that entails lifestyle changes, therapy, or potential use of devices to monitor and improve your sleep.
Next Steps After Receiving Your Results
After discussing your results, your doctor may suggest various treatments or further testing. If a condition like sleep apnea is diagnosed, options may include CPAP therapy, lifestyle alterations, or even oral appliances. Conversely, if results point to insomnia or other non-apnea related issues, behavioral therapies or sleep hygiene education could be recommended.
In any case, knowing what your sleep study results mean and what actions to take can significantly impact your overall health and well-being. Don’t hesitate to reach out for support and guidance as you take these important steps to enhance your sleep quality and health.
Common Sleep Disorders Diagnosed by Sleep Studies
Sleep studies serve as a pivotal tool in diagnosing a variety of sleep disorders that can significantly impact your overall health and well-being. Understanding these disorders is essential for seeking appropriate treatment and improving your quality of life. Among the most common conditions diagnosed through sleep studies are sleep apnea, insomnia, and restless legs syndrome, each of which presents unique challenges and symptoms.
Sleep apnea, characterized by repeated interruptions in breathing during sleep, is a leading diagnosis from sleep studies. It can manifest in two primary forms: obstructive and central sleep apnea. Obstructive sleep apnea occurs when throat muscles intermittently relax and block the airway, while central sleep apnea happens when the brain fails to send appropriate signals to the muscles that control breathing. Diagnosing sleep apnea typically involves monitoring the frequency of apneas and hypopneas, which can be quantified through metrics like the Apnea-Hypopnea Index (AHI) recorded during a polysomnography sleep study.
Insomnia-a prevalent condition where individuals struggle to fall asleep or stay asleep-can also be assessed during a sleep study. The data collected often reveals patterns of wakefulness, the total sleep time, and disturbances, allowing professionals to distinguish between primary insomnia and insomnia linked to other health issues. Behavioral therapies and improvements in sleep hygiene are commonly recommended following a diagnosis.
Restless legs syndrome (RLS) causes an irresistible urge to move the legs, typically accompanied by uncomfortable sensations. This condition can significantly disrupt sleep, leading to daytime fatigue. Sleep studies can help identify RLS by monitoring the movements and symptoms that occur during the night, enabling doctors to devise effective treatment plans that may include lifestyle changes or medications.
In addition to these disorders, sleep studies can pinpoint other conditions such as narcolepsy, periodic limb movement disorder, and parasomnias (which include activities like sleepwalking). Knowing the specific disorder is crucial, as it directly informs the course of treatment and lifestyle modifications that can enhance sleep quality.
By understanding these common sleep disorders and how they are diagnosed, you empower yourself to seek appropriate interventions. Remember, effective sleep health management begins with awareness and proper guidance from qualified health professionals.
At-Home Sleep Studies vs. In-Lab Studies: Pros and Cons
Many patients find themselves weighing the options of at-home sleep studies versus traditional in-lab studies when it comes to diagnosing sleep disorders. Each method has distinct advantages and drawbacks that can significantly impact the effectiveness of diagnosis and the patient experience.
At-Home Sleep Studies
At-home sleep studies, typically conducted using portable monitoring devices, offer a more convenient option for many individuals. Since these studies are performed in the comfort of one’s home, patients often feel more relaxed, which can lead to more accurate readings of natural sleep patterns. The equipment is usually user-friendly, allowing patients to set up the devices with minimal assistance.
However, at-home studies may have limitations. They generally monitor fewer parameters compared to in-lab studies, which can result in less comprehensive data. For instance, while they effectively track fundamental metrics like breathing patterns and oxygen levels, they may not capture other essential factors such as brain activity, which is crucial for diagnosing complex disorders like narcolepsy. This streamlined approach may be adequate for conditions like obstructive sleep apnea but could miss nuances in more complicated cases.
In-Lab Sleep Studies
Conversely, in-lab sleep studies, or polysomnography, offer a thorough examination of sleep. Conducted overnight in a sleep center, these studies provide comprehensive data, including brainwave activity, heart rate, respiratory events, and muscle activity. This extensive monitoring makes in-lab studies the gold standard for diagnosing a wide array of sleep disorders.
Despite their thoroughness, in-lab studies can be intimidating. The unfamiliar environment, coupled with wires and sensors attached to the body, may disrupt some patients’ ability to sleep comfortably. Additionally, in-lab tests are often more expensive and might involve a longer wait for scheduling and insurance approvals.
Weighing the Options
When choosing between at-home and in-lab studies, patients should consider several factors:
- Comfort: If you feel more at ease at home, an at-home study might yield better results.
- Diagnosis complexity: For more complex disorders, an in-lab study may provide the thorough analysis required.
- Cost: Review insurance coverage and personal budgets to determine what’s feasible.
- Time: Consider how quickly you need results; in-lab studies may have longer wait times.
Real-world scenarios can help clarify the decision. For example, a patient with difficulty breathing at night may benefit from an at-home study to screen for sleep apnea. Conversely, someone experiencing severe daytime sleepiness and other symptoms indicative of narcolepsy would likely need the detailed data that only an in-lab study can provide.
In summary, understanding the pros and cons of each type of sleep study allows patients to make informed decisions tailored to their specific health needs and personal circumstances.
Insurance Coverage and Costs of Sleep Studies
Navigating the costs and insurance coverage for sleep studies can feel overwhelming, especially when you’re trying to prioritize your health. Typically, the expenses associated with sleep studies can vary significantly based on your location, the type of study (in-lab or at-home), and the specific tests performed. On average, in-lab sleep studies-often considered the gold standard-can range from $1,000 to $3,000, depending on the complexity and the facility’s pricing. In contrast, at-home sleep studies are generally more affordable, typically costing between $150 and $500.
Insurance coverage plays a crucial role in determining how much of this cost you might bear. Many insurance plans do cover sleep studies, especially if you have a history of sleep disorders or symptoms signaling such issues. It’s essential to check with your provider before scheduling a study. Ask about your specific plan’s coverage, including any co-pays or deductibles that might apply. Getting pre-authorization from your insurance company is highly advisable, as it can help avoid unexpected expenses later on.
Tips for Navigating Insurance and Costs
To make the process smoother, consider these practical steps:
- Contact your insurance provider: Start by calling the number on your insurance card. They can provide detailed information regarding coverage for sleep studies, including which facilities are in-network.
- Inquire about pre-authorization: Many insurers require pre-approval for sleep studies. Confirm whether this is necessary to avoid incurring out-of-pocket costs.
- Request an itemized bill: If you end up having a sleep study, ask for an itemized bill to ensure that you’re being charged correctly and to help clarify what portions may be covered by insurance.
- Explore payment plans: If you discover that a sleep study is outside your budget, don’t hesitate to discuss payment plans with the provider’s office. Many facilities offer financing options to help alleviate the financial burden.
Being proactive in understanding your insurance coverage and the costs associated with sleep studies can empower you to make an informed decision about your health. Remember, prioritizing your sleep is often a crucial step in improving overall well-being, so don’t let financial concerns hold you back from seeking the help you need.
Emerging Technologies in Sleep Monitoring
are revolutionizing how we understand and address sleep health. As awareness of sleep’s critical role in overall well-being grows, so do the innovations aimed at improving sleep quality and diagnosing potential disorders. One of the most significant advances is the development of wearable devices that can track sleep patterns in real-time. Many of these consumer-grade gadgets, like smartwatches and fitness bands, employ sensors to collect data on heart rate, movement, and even blood oxygen levels, giving users valuable insights into their sleep cycles without the need for an overnight stay in a sleep lab.
At-Home Sleep Monitoring Devices
At-home devices have been designed to offer a more accessible way to monitor sleep without the anxiety often associated with traditional sleep studies. These devices typically utilize advanced technology, such as actigraphy and pulse oximetry, to assess sleep quality. For instance, the Oura Ring and Fitbit provide users with detailed reports about sleep stages, duration, and even disturbances during the night. Such insights can empower individuals to make informed lifestyle changes to improve their sleep hygiene.
Emerging Technologies in Sleep Studies
On the clinical side, researchers are increasingly utilizing more sophisticated technologies like polysomnography (PSG), which records brain waves, oxygen levels, heart rate, and breathing, as well as eye and leg movements during sleep. Advances in artificial intelligence (AI) are allowing for more accurate data analysis from these studies, helping healthcare providers interpret complex patterns quickly and efficiently. Additionally, remote monitoring technologies enable doctors to analyze data captured during sleep studies from the comfort of their own offices, enhancing convenience for both patients and providers.
Wearable Tech versus Traditional Methods
While wearables offer a host of advantages, they also come with limitations. Many devices do not provide a comprehensive analysis needed for a definitive sleep disorder diagnosis. For serious concerns, especially symptoms like severe sleep apnea or narcolepsy, a traditional sleep study may still be necessary. In general, it’s wise to view wearables as helpful tools for tracking trends rather than replacements for professional assessments.
- Wearable Devices: Convenient and user-friendly, good for tracking general sleep patterns.
- In-Lab Studies: Offer comprehensive analysis and diagnosis; considered the gold standard.
- Telehealth Monitoring: More providers are adopting remote monitoring options for follow-up on sleep conditions.
As technology continues to advance, the future of sleep monitoring looks promising. Increased accessibility to accurate sleep data can lead to better management of sleep health, enabling individuals to take proactive steps towards improving their sleep quality. With the right tools and knowledge, navigating your sleep health has never been easier.
When to Seek Help: Knowing Your Sleep Health
Recognizing when to seek help for sleep-related issues is crucial. Sleep is often overlooked, yet it plays a vital role in overall health and well-being. If you find yourself consistently struggling to fall asleep, stay asleep, or wake up too early, it may be time to consult a healthcare professional. Persistent fatigue, difficulty concentrating, or falling asleep during the day are strong indicators that your sleep health may need attention.
A good place to start is by monitoring your sleep patterns using a sleep diary or wearable devices. These tools can provide insights into sleep duration, quality, and disturbances, helping you track annoying trends over time. If you’re noticing significant changes or ongoing difficulties, it often signals a need for more in-depth analysis. Additionally, if you experience symptoms like gasping for air during sleep, loud snoring, or extreme mood fluctuations, these may point to sleep disorders such as sleep apnea or insomnia, which necessitate further evaluation.
When considering testing options, understanding the difference between at-home and in-lab studies is vital. At-home tests can be convenient and less intimidating, but they may not capture all the necessary data for a precise diagnosis. In contrast, a comprehensive in-lab sleep study allows for a complete assessment using polysomnography (PSG), which monitors various physiological signals and provides valuable insights into your sleep architecture.
If your initial steps with tracking or even minor adjustments to your sleep routine don’t yield improvements, don’t hesitate to reach out for professional help. Early intervention can lead to better outcomes, helping you reclaim the restorative sleep your body needs.
Frequently asked questions
Q: What are common sleep disorders diagnosed by sleep studies?
A: Common sleep disorders diagnosed by sleep studies include obstructive sleep apnea, insomnia, and narcolepsy. Each disorder impacts sleep quality and overall health differently, making accurate diagnosis essential. Understanding these conditions can help improve sleep health. For more insights on sleep disorders, visit our section on common sleep disorders.
Q: How long does a typical sleep study take?
A: A typical sleep study, or polysomnography, takes about 6 to 8 hours. It usually begins in the evening and lasts through the night. This duration allows enough time to monitor various sleep stages and patterns. For a detailed walkthrough of what happens, see our step-by-step process section.
Q: What can I do to prepare for a sleep study?
A: To prepare for a sleep study, avoid caffeine and alcohol the day before, and maintain your regular sleep schedule. Wear comfortable clothing and bring any personal items needed for a good night’s sleep. For more tips, check the “Preparing for Your Sleep Study” section.
Q: Will my sleep study be covered by insurance?
A: Often, insurance does cover sleep studies, especially when referred by a healthcare provider for suspected sleep disorders. It’s advisable to check with your insurance provider regarding coverage specifics. Explore our section on insurance coverage and costs for more detailed guidance.
Q: Can I perform a sleep study at home?
A: Yes, at-home sleep studies are available and can be suitable for certain conditions like sleep apnea. They are less comprehensive than in-lab tests but can effectively diagnose some sleep disorders. Compare your options further in our At-Home Sleep Studies vs. In-Lab Studies section.
Q: What technology is used in sleep studies?
A: Sleep studies utilize various technologies including polysomnography, which records brain waves, oxygen levels, heart rate, and breathing activities. Newer options may involve wearable devices for home monitoring. For emerging technologies, see our section on Emerging Technologies in Sleep Monitoring.
Q: How are sleep study results interpreted?
A: Sleep study results are interpreted by sleep specialists who analyze various metrics such as sleep stages and interruptions. A report will typically detail any diagnosed conditions. For a straightforward breakdown, refer to our interpreting sleep study results guide.
Q: What should I expect during the night of a sleep study?
A: During the night of a sleep study, you’ll be monitored while you sleep, and sensors will record your body’s activity. It’s typically held in a comfortable room to minimize anxiety. Learn more about what to expect during your sleep study night in our dedicated section.
Closing Remarks
Now that you understand the step-by-step process of how sleep studies are performed, it’s time to take control of your sleep health. Remember, addressing sleep disorders can significantly enhance your well-being, making it crucial to consult with your healthcare provider if you suspect an issue. For more information, consider exploring our comprehensive resources on diagnosing sleep apnea or download our handy products page for sleep aids and technologies designed to enhance your nightly rest. Join the conversation by sharing your experiences or questions in the comments below-your journey could inspire others! Keep exploring our site to empower yourself with knowledge and practical tips that will help you achieve the restorative sleep you deserve.