Navigating the world of sleep apnea treatment can be overwhelming, especially when it comes to understanding whether a sleep study is necessary for obtaining a CPAP machine. Approximately 22 million Americans suffer from sleep apnea, and many experience symptoms like excessive daytime fatigue or snoring. A sleep study, or polysomnography, is often the first step to diagnose this condition, enabling doctors to prescribe appropriate treatments. However, there are alternative pathways to access CPAP therapy that could save time and reduce anxiety. This article will clarify the rules surrounding sleep studies and the circumstances under which you might still qualify for a CPAP without one. By the end, you’ll be empowered to make informed decisions about your sleep health and treatment options.
Do You Need a Sleep Study for CPAP? Understanding the Basics
Sleep apnea is a silent yet significant disruptor of health, affecting millions of people globally. One of the most effective treatments for this disorder is Continuous Positive Airway Pressure (CPAP) therapy. However, before starting CPAP, it’s crucial to understand how a sleep study plays a foundational role in diagnosing sleep apnea and determining the appropriate treatment. Though some might wonder if a sleep study is necessary for obtaining a CPAP machine, the guidance is clear: a sleep study is often essential for accurate diagnosis.
A sleep study, medically known as polysomnography, evaluates your sleep patterns comprehensively. It monitors critical factors such as brain waves, heart rate, breathing, and oxygen levels during sleep. This thorough analysis helps your healthcare provider confirm whether you have sleep apnea and the severity of the condition. In essence, having a properly conducted sleep study can ensure that the prescribed CPAP therapy is tailored to your specific needs, optimizing your chances for effective treatment and better sleep quality.
Both in-lab and home sleep tests are available options, with each method having its benefits depending on your situation. Home sleep tests can offer convenience and comfort, often capturing essential data while you sleep in your own bed. However, they may not be suitable for everyone, especially those with complex sleep disorders. On the other hand, in-lab studies provide a comprehensive evaluation but can be more time-consuming and intimidating due to the clinical environment.
Understanding whether a sleep study is needed might seem daunting, but the process is structured to ensure you receive the best care. If you exhibit symptoms like loud snoring, gasping for air during sleep, or excessive daytime fatigue, it’s advisable to consult a healthcare professional about undergoing a sleep study. This initial step sets you on the right path toward effective management of sleep apnea and enhances your overall health and well-being.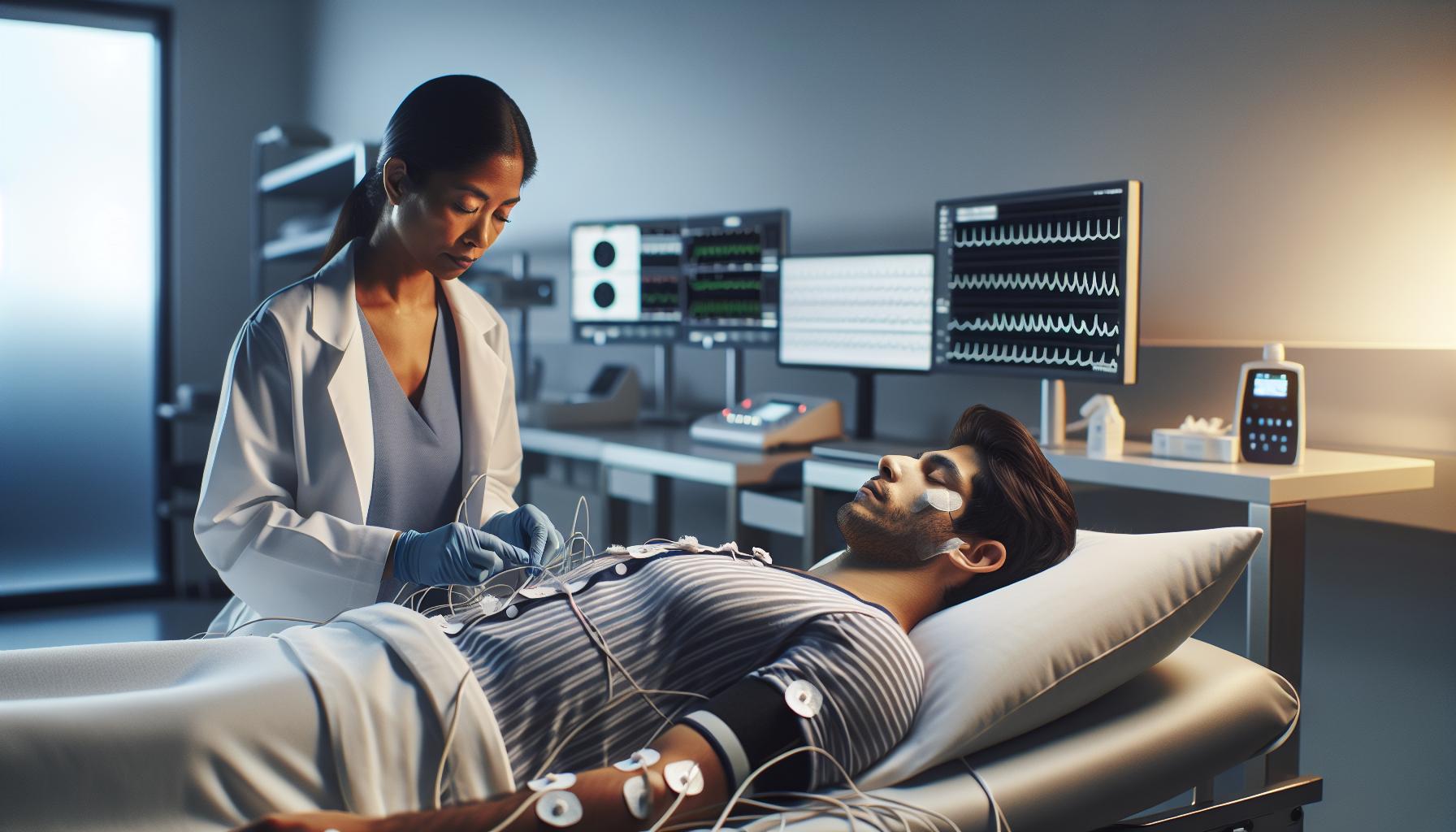
The Importance of Sleep Studies for Sleep Apnea Diagnosis
A sleep study is often the essential first step in diagnosing sleep apnea, paving the way for effective treatment decisions. This comprehensive evaluation, known as polysomnography, provides critical insights into your sleep patterns by monitoring key physiological functions such as brain activity, heart rate, and oxygen levels. It’s more than just counting how long you sleep; it’s about understanding the quality of your sleep and identifying any disruptions that could lead to health issues if left untreated.
Many people suffering from sleep apnea might not be fully aware of their condition. Symptoms such as loud snoring, choking during sleep, or daytime fatigue can easily go unnoticed until they significantly impact your quality of life. A sleep study not only helps in confirming the diagnosis but also determines the severity of the condition, which is vital for tailoring the most effective CPAP therapy. In short, understanding the severity allows physicians to adjust therapy settings accordingly, which can significantly improve comfort and outcomes for patients.
The fear of undergoing a sleep study often stems from misinformation. It’s important to know that modern sleep studies are designed to be as non-intrusive and comfortable as possible. If you’re considering a sleep study, here’s what you can expect:
- Preparation: You’ll receive guidelines on how to prepare for the test, including any medications to avoid and what to bring.
- During the Study: Sensors will be placed on your body, usually without any pain, to gather important data. You’ll be monitored overnight while you sleep, either in a lab or at home with a portable device.
- Post-Study: The data will be analyzed by a sleep specialist who will then discuss the results and your treatment options.
As you weigh whether to undergo a sleep study, remember that it’s a tool for empowerment rather than an obstacle. The information gained can lead to better sleep, enhanced health, and improved daily functioning. Seeing the process from this perspective can alleviate anxieties and highlight the benefits of taking charge of your sleep health.
What to Expect During a Sleep Study: A Step-by-Step Guide
Imagine slipping into a cozy bed, the soft hum of technology working for you, gathering insights into a world you can’t consciously monitor-your sleep. This is what a sleep study, or polysomnography, offers; it’s your chance to unveil the mysteries of your nighttime habits, critical if you’re considering CPAP therapy. Knowing what to expect can turn anxiety into empowerment, transforming a daunting process into a valuable journey toward improved health.
Preparing for your sleep study typically begins with clear instructions from your healthcare provider. You may be advised to avoid caffeine and certain medications for a couple of days prior. If the study is conducted at a sleep center, remember to pack comfortable sleepwear and any personal items that make you feel at ease. If you’re undergoing a home sleep test, gather the equipment from your provider, which may include a monitoring device and sensors that track vital signs.
On the night of the study, expect a comfortable environment. In a sleep laboratory, you’ll find a private room, often more like a hotel suite than a hospital. Technicians will place painless sensors on your scalp, face, chest, and legs to monitor brain waves, heart rate, and breathing patterns. You’ll be asked to sleep as you normally would, allowing the equipment to record how you progress through different sleep stages, including REM and deep sleep.
After the study, the collected data is analyzed by a sleep specialist who will interpret the results, helping you understand the underlying factors affecting your sleep. Should it reveal sleep apnea or another disorder, it will help guide the necessary adjustments to initiate effective CPAP treatment if indicated. Understanding this process not only demystifies sleep studies but also empowers you to take control of your sleep health, equipping you with knowledge that can significantly enhance your quality of life.
Alternative Options: Home Sleep Tests versus In-Lab Studies
When it comes to diagnosing sleep disorders, especially sleep apnea, individuals often face a crucial decision: should you undergo a home sleep test or an in-lab study? Each option presents unique benefits and considerations that can greatly influence your comfort, convenience, and the accuracy of the results.
Home sleep tests provide a more convenient, cost-effective way to monitor your sleep in the comfort of your own bed. These tests involve wearing a portable monitoring device that tracks your breathing, heart rate, and blood oxygen levels while you sleep. The setup is generally straightforward, requiring you to attach sensors to your body and follow simple instructions. This option can be especially appealing for those who are anxious about sleeping in a lab environment or who have a busy schedule. However, home tests may not capture all the nuances of your sleep stages or identify other complex sleep disorders. They are primarily designed to diagnose moderate to severe obstructive sleep apnea, meaning if your results are inconclusive, further testing may still be required.
On the other hand, in-lab studies, or polysomnography, offer a comprehensive evaluation. Conducted overnight in a specialized sleep center, these studies monitor a wide range of physiological functions, including brain activity, muscle tone, and eye movements in addition to traditional metrics like heart rate and oxygen levels. This setting allows for a deeper understanding of your sleep patterns and can differentiate between various sleep disorders, not just sleep apnea. While in-lab studies can be more expensive and involve some discomfort from the sensors and environment, they provide a thorough assessment which can lead to more precise treatment decisions.
Ultimately, the choice between a home sleep test and an in-lab study comes down to personal preference and the recommendations of your healthcare provider. If you have simpler symptoms that align closely with obstructive sleep apnea, a home test may suffice. Conversely, if you exhibit more complex symptoms or if previous tests were inconclusive, an in-lab study may be warranted. It’s essential to consult with a sleep specialist who can guide you toward the option that best meets your health needs and ensures accurate diagnostics for effective CPAP therapy or other treatments.
Navigating Insurance: Will Your Plan Cover a Sleep Study?
Navigating insurance coverage for a sleep study can feel overwhelming, but understanding your policy can significantly ease the process. Many people are surprised to learn that insurance plans often cover sleep studies, particularly when they are deemed medically necessary. However, coverage can vary widely depending on your provider and the specifics of your plan, so it’s essential to double-check your benefits.
Start by contacting your insurance company to confirm whether they cover sleep studies and under what circumstances. Ask specifically about the types of studies covered-such as home sleep tests versus in-lab polysomnography-and any requirements for pre-authorization that may apply. Some plans may require a referral from your primary care physician or documentation of symptoms consistent with sleep apnea before they will approve coverage.
It’s also wise to inquire about your out-of-pocket costs. Some insurance plans may cover the entire study, while others may have co-pays, deductibles, or co-insurance that could impact your overall expenses. Understanding these details upfront can help you prepare for any financial responsibilities you may face.
When discussing your insurance with your doctor or sleep specialist, be sure to mention any previous diagnoses or treatments related to sleep apnea. This information can help strengthen the case for necessity, making it more likely that your insurance will approve your request. Remember to keep a detailed record of all communications with your insurance provider, as this documentation can be invaluable if any disputes arise later on regarding coverage or billing.
In conclusion, being proactive about understanding your insurance coverage for sleep studies is a critical step towards effective sleep apnea management. By knowing what to ask and documenting your interactions, you can relieve much of the stress associated with insurance processes and focus on finding the right treatment for your sleep health.
Real-World Scenarios: When to Seek a Sleep Study
Many people underestimate the importance of a proper diagnosis when it comes to sleep apnea. If you’re struggling with frequent snoring, excessive daytime fatigue, or waking up gasping for air, it may be time to consider a sleep study. These scenarios are often indicators of sleep apnea, a serious condition that disrupts your sleep cycle and overall health. Understanding when to seek a sleep study can empower you to take control of your sleep health.
In situations where lifestyle changes-like weight loss or changing sleep positions-aren’t effective, a sleep study is often the next logical step. For instance, if you’ve tried elevating your head while sleeping or adopting a healthier diet, yet continue to experience inadequate sleep, this could signal a need for a more thorough investigation into your sleep patterns. A sleep study, conducted in a lab or at home, can provide essential data by monitoring factors such as your breathing, heart rate, and oxygen levels during sleep.
Consider the following scenarios where seeking a sleep study is warranted:
- Chronic Fatigue: If you find yourself feeling excessively tired despite getting the recommended 7-9 hours of sleep, a sleep study can help determine if there’s an underlying issue.
- Frequent Nighttime Interruptions: Waking up multiple times throughout the night, especially with gasping or choking sensations, is a clear sign to seek medical advice and possibly a sleep study.
- Bed Partner Concerns: If a partner has mentioned loud snoring or observed you stop breathing during sleep, these accounts can corroborate your symptoms and warrant a study.
It’s also essential to communicate openly with your healthcare provider. If they suspect sleep apnea based on your symptoms and possibly a sleep questionnaire, they can recommend the appropriate tests. Remember, sleep studies not only aid in diagnosing sleep apnea but also help tailor treatment options like CPAP therapy, ensuring you receive the most effective care for your needs.
How Wearable Devices Compare to Sleep Studies
Wearable devices are increasingly popular for tracking sleep patterns and health metrics, but how do they stack up against traditional sleep studies for diagnosing sleep apnea? While wearables offer accessible and convenient ways to gather data about your sleep, they have limitations that are important to understand if you suspect you have a sleep disorder.
Wearable devices typically monitor metrics like heart rate, movement, and sometimes even oxygen saturation. They can give you insights into your overall sleep quality, including how long you spend in various sleep stages and how often you wake up during the night. This data can be quite helpful, especially for individuals looking to improve their sleep hygiene or simply gain a better understanding of their nightly rest patterns.
However, despite their convenience, these devices fall short when it comes to providing comprehensive diagnostics. Sleep studies, which can be in-lab polysomnography or home sleep apnea tests, are conducted under controlled conditions and measure a range of physiological parameters, including brain activity, breathing patterns, and muscle tone, that wearables cannot accurately assess. This detailed analysis is crucial for diagnosing conditions like sleep apnea, where the precise nature of breathing disruptions is key to determining the best treatment options.
In practical terms, if you’re experiencing symptoms like frequent daytime fatigue or loud snoring, a sleep study is likely your best course of action. While wearables can track trends and help you notice patterns, they cannot definitively diagnose sleep apnea. They may, however, serve as a useful preliminary tool to assist in discussions with your doctor regarding whether a sleep study is necessary. For those who have tried lifestyle changes without improvement, seeking a sleep study can provide clarity and lead to an effective treatment plan tailored to your specific needs.
In conclusion, while wearable devices can offer valuable insights into your sleep habits, they should not replace professional sleep studies, especially if you suspect you have sleep apnea. Understanding the strengths and weaknesses of both approaches is essential in navigating your sleep health journey.
Setup and Usage of CPAP Machines After a Sleep Study
Getting accustomed to a CPAP (Continuous Positive Airway Pressure) machine can significantly improve your quality of sleep after a sleep study confirms a diagnosis of sleep apnea. The journey from diagnosis to effective usage of a CPAP machine involves several important steps, each aimed at ensuring that you benefit fully from this therapy in managing your condition.
First, understanding how to set up your CPAP machine is crucial. Most devices come with a clear set of instructions, but generally, you’ll need to follow these steps:
- Assemble the components: Connect the mask to the tubing, ensuring that all connections are secure.
- Add water if required: If your machine has a humidifier, fill it with distilled water to avoid mineral buildup.
- Power on the machine: Plug in your CPAP machine and adjust the settings as instructed by your healthcare provider.
- Fit the mask properly: Adjust the straps of your mask for a snug fit, ensuring that it’s comfortable yet secure enough to prevent air leaks.
Next, familiarizing yourself with the CPAP settings is essential. Your doctor will likely adjust the pressure settings based on the severity of your sleep apnea, which might require some personal tuning to ensure comfort. If the pressure feels too high or low, discuss recalibrating it with your healthcare team.
Using the CPAP machine consistently can take time to adjust to. Here are some tips to help you adapt:
Getting Comfortable with CPAP Usage
- Establish a Routine: Try to wear your CPAP machine every night, even if it feels uncomfortable at first. Consistency is key to getting used to it.
- Practice During the Day: Wearing your mask while awake can help you become accustomed to the sensation of it.
- Explore Mask Options: If your initial mask choice isn’t comfortable, consult with your doctor about alternatives. There are nasal masks, full-face masks, and even pillow masks, allowing a fit that suits your preferences.
Troubleshooting Issues
If you encounter problems-like excessive air leaks, dry mouth, or difficulty getting to sleep-there are several strategies to consider:
- Air Leaks: Adjust the mask fit or try a different size. Using a chin strap might help keep your mouth closed if you’re a mouth breather.
- Dry Mouth: If you experience dryness due to the CPAP, try using a heated humidifier attached to your device.
- Difficulty Sleeping: Gradually increase the amount of time you wear the CPAP each night to make acclimatization easier.
Adopting a CPAP machine is a significant step towards controlling sleep apnea and improving your overall health. Stay in regular contact with your healthcare provider to share your experiences, as they can offer support and adjustments to your treatment plan, enhancing your journey to restful sleep.
Troubleshooting Common Issues with CPAP Therapy
Adjusting to a CPAP (Continuous Positive Airway Pressure) machine can sometimes feel overwhelming, but knowing how to troubleshoot common issues can make the transition smoother. Many new users encounter challenges that can detract from their therapy experience. However, with the right strategies, you can overcome these obstacles and enjoy the revitalizing benefits of restful sleep.
One frequent issue that users face is air leaks. These leaks can occur when the mask does not fit properly, leading to discomfort and ineffective therapy. If you’re experiencing this problem, start by checking the mask’s fit. If it’s snug but still leaking, consider adjusting the straps or trying a different mask size or style. A chin strap can also be a helpful addition to keep your mouth closed if you tend to breathe through your mouth while sleeping.
Another common complaint is dry mouth, especially for users who breathe through their mouths. This can be especially annoying at night, impacting your sleep quality. To alleviate this discomfort, you might try using a heated humidifier with your CPAP machine. This addition enriches the air with moisture, helping to prevent dryness in your mouth and throat. Ensuring that the humidifier is filled with distilled water can also help avoid mineral buildup that could affect performance.
Finally, some users have difficulty falling asleep or staying asleep while using their CPAP machines. If you find yourself tossing and turning, consider gradually increasing the amount of time you wear your CPAP machine each night. Start with short sessions during the day while watching TV or relaxing, and progressively extend this time to help your body acclimate to the mask and pressure. Practicing relaxation techniques before bedtime, such as deep breathing exercises or gentle stretches, can also help ease you into sleep more comfortably.
With patience and the right approaches, you can effectively address common issues associated with CPAP therapy. Regular communication with your healthcare provider is vital-they can provide personalized advice and adjustments to your treatment plan, support you in overcoming any challenges, and ultimately enhance your journey to more restful sleep.
Exploring Other Treatments for Sleep Apnea Beyond CPAP
Exploring effective alternatives to CPAP therapy can provide individuals with sleep apnea greater flexibility and comfort. While CPAP machines are prevalent and effective, they are not the only option available. Understanding these alternatives can empower patients in their treatment decisions.
Oral Appliances
Oral appliances, often custom-made by dentists specializing in sleep medicine, are designed to reposition the jaw and keep the airway open during sleep. They are particularly useful for those with mild to moderate obstructive sleep apnea (OSA) and can be more comfortable for patients who struggle with CPAP masks. Many users find them less invasive and easier to tolerate than CPAP therapy. It’s essential to consult a dental professional who can provide a proper fitting and follow-up care to ensure effectiveness.
Positional Therapy
For some individuals, sleep position plays a significant role in the severity of apnea events. Positional therapy involves techniques to encourage sleeping on one’s side rather than the back, as this can often reduce the frequency and severity of apneas. Specialized pillows or wearable devices that vibrate when the user shifts to a supine position can be helpful. Not only is this method non-invasive, but it can also be easily incorporated into a sleep routine.
Behavioral and Lifestyle Changes
Adopting a healthier lifestyle can significantly impact sleep apnea symptoms. Weight loss is particularly effective for those who are overweight, as reducing body fat can minimize airway obstruction. Additionally, avoiding alcohol and sedatives before bedtime, quitting smoking, and establishing a regular sleep schedule are vital steps. Each of these changes supports overall health while reducing the severity of sleep apnea.
Surgical Options
For patients with anatomical abnormalities contributing to their apnea, surgical interventions may prove beneficial. Various procedures can remove excess tissue from the throat or reposition anatomical structures to improve airflow. If conservative treatments fail, a consultation with an ENT specialist can help patients understand the risks and benefits associated with surgical options.
Through understanding these alternatives, individuals can take a more active role in their treatment plans. Discussing these options with healthcare providers can lead to personalized strategies that better suit their needs and lifestyles, potentially leading to better compliance and improved sleep quality.
User Experiences: Success Stories with Sleep Studies and CPAP
Many individuals facing sleep apnea find solace in the success stories of others who have undergone sleep studies and found effective treatments like CPAP (Continuous Positive Airway Pressure) therapy. These experiences can provide encouragement, illustrating that while the path to better sleep might involve initial anxiety and uncertainty, it often leads to transformational benefits in health and quality of life.
Consider the journey of Mike, a middle-aged man who had been struggling with excessive daytime sleepiness and loud snoring for years. Initially, he hesitated to pursue a sleep study due to fears about the unfamiliarity of the testing process. However, after discussing his symptoms with a healthcare provider, he decided to proceed with the study. The results confirmed he had obstructive sleep apnea, prompting the recommendation of a CPAP machine. Experiences shared in support groups revealed to Mike that many users had similar apprehensions and that CPAP therapy could significantly improve energy levels and overall well-being.
The setup of his CPAP machine turned out to be straightforward, thanks in part to instructional videos and guides from his sleep specialist that demystified the process. Mike also discovered the importance of adjusting the machine settings to suit his needs, and within a few weeks, he experienced better sleep quality. His friends and family noticed the positive change; he was more alert and engaged in conversations, reclaiming joy in everyday activities.
Stories like Mike’s highlight the real-world impact of understanding sleep apnea and the effectiveness of CPAP therapy. Many users testify that the initial discomfort of wearing a mask is easily outweighed by the substantial improvements in their health and wellness. It’s not just about sleeping better; it’s about living better. Regular follow-ups with sleep specialists also help ensure that the device remains effective and allows for adjustments based on changing needs.
Ultimately, these success stories amplify the message that seeking a sleep study can be an empowering step toward reclaiming one’s health. With a supportive healthcare team and community behind them, individuals can overcome their fears, find the right treatment, and embark on a journey toward restorative sleep. If you’re grappling with symptoms of sleep apnea, remember-anxiety about the process is common, but the benefits can far exceed the initial hurdles.
Expert Opinions: Sleep Specialists Weigh In on Testing Necessity
Sleep specialists emphasize the critical role of sleep studies in accurately diagnosing conditions like sleep apnea before starting treatments such as CPAP (Continuous Positive Airway Pressure) therapy. Experts argue that a formal diagnosis through a sleep study is essential for tailoring effective treatment strategies. According to Dr. Emily Chang, a board-certified sleep medicine physician, “Relying solely on symptoms can lead to misdiagnosis and inappropriate treatment.” Therefore, getting a sleep study offers a clearer picture of how your body behaves during sleep, enabling clinicians to assess severity and devise a personalized management plan.
Why Testing is Crucial
Sleep studies provide invaluable data, capturing information about breathing patterns, oxygen levels, and overall sleep quality through polysomnography. This diagnostic tool can help uncover not only obstructive sleep apnea but other potential sleep disorders as well. For example, Dr. Mark Harrison of the Sleep Disorders Center notes, “We often discover comorbid conditions that would otherwise go unnoticed without comprehensive testing.” Identifying these issues is vital because treatment success hinges on understanding the complete clinical context, thus enhancing the likelihood of a positive response to CPAP therapy.
The Role of Home Sleep Tests
In recent years, home sleep tests (HST) have gained traction as a more convenient alternative for diagnosing sleep apnea. While HSTs can be effective for many individuals, sleep specialists caution that they aren’t a one-size-fits-all solution. Dr. Lisa Gomez, a renowned sleep researcher, points out, “Home tests can miss more complex disorders or fail to provide the full spectrum of sleep data.” Therefore, for those with more complicated symptoms or risk factors, an in-lab sleep study may still be necessary. The combination of accessibility and comprehensive data is essential for effective treatment.
Addressing Anxiety Around Testing
It is natural to feel anxious before undergoing a sleep study. However, specialists like Dr. Chang reassure patients that the procedure is straightforward and significantly beneficial. “Understanding that these tests are designed to help you is crucial. You’ll be monitored in a comfortable environment, and the data collected will empower us to find the best treatment for you,” she advises. This reassurance can ease the apprehension surrounding sleep studies, encouraging more individuals to seek help for their sleep issues.
In sum, while sleep studies might seem daunting at first, they are a vital step toward understanding and addressing sleep disorders effectively. Engaging with sleep specialists provides not only peace of mind but also the critical guidance needed for improved sleep health.
Faq
Q: Do I need a prescription for a CPAP machine?
A: Yes, a prescription is required to obtain a CPAP machine legally. This ensures the device is tailored to your specific needs based on the results of a sleep study. Consult with a healthcare provider or sleep specialist for proper evaluation.
Q: What are the alternatives to a traditional sleep study?
A: Alternatives to traditional sleep studies include home sleep testing. These tests are typically less invasive and can often be completed in your own bed. However, they may not capture as much data as an in-lab study. Check the full comparison in our article’s section on alternative options.
Q: How long does a sleep study take?
A: A standard sleep study typically takes one night, but some tests may require multiple nights for comprehensive data collection. Expect to be at the sleep center for several hours, including setup time. For more details on what to expect, refer to the sleep study guide in our article.
Q: Can I use a CPAP without a sleep study if I suspect sleep apnea?
A: While some people may want to self-treat, using a CPAP machine without a proper diagnosis from a sleep study is not advisable. It’s essential to have a healthcare professional evaluate your symptoms and confirm the necessity of CPAP therapy for effective treatment.
Q: What should I bring to a sleep study?
A: Bring comfortable sleepwear, toiletries, any medications you take, and items that help you relax. It’s important to familiarize yourself with the environment to ensure a restful night. For more tips, you can check the section on what to expect during a sleep study.
Q: How do sleep studies impact insurance coverage for CPAP?
A: Many insurance plans require a documented sleep study before they will cover CPAP equipment. It’s important to understand your specific plan and discuss this with your provider to avoid unexpected costs. Refer to the insurance navigation section of our article for more insights.
Q: Are sleep studies the only way to diagnose sleep apnea?
A: While sleep studies are the gold standard for diagnosing sleep apnea, other methods such as home sleep tests or questionnaires might provide useful information. However, a comprehensive sleep study is the most reliable for diagnosis. Explore more about this in the related sections of our article.
Q: What if my sleep study results are inconclusive?
A: If your sleep study results are inconclusive, your doctor may recommend further testing or alternative evaluation methods. It’s essential to follow up with your healthcare provider for the next steps. Detailed guidance on this is available in our real-world scenarios section.
The Conclusion
In conclusion, understanding whether a sleep study is necessary for obtaining a CPAP is crucial for taking control of your sleep health. If you’re experiencing symptoms of sleep apnea, don’t hesitate-consider scheduling a sleep study to get the insights you need. For further exploration, check out our detailed guide on the costs and expectations of sleep studies, and learn how sleep technology like wearables can complement your health journey.
Your sleep matters, and the sooner you take action, the better your quality of life can become. Have questions? Comment below or connect with our community for support. And don’t forget to sign up for our newsletter for more tips on improving your sleep health and staying informed about the latest in sleep technology. Together, we can help you navigate your path to restful nights!