Did you know that nearly 70 million Americans struggle with sleep disorders, making understanding sleep studies vital for improving health? A sleep study, also known as polysomnography, is a comprehensive evaluation used to diagnose various sleep issues by monitoring brain activity, heart rate, and breathing patterns while you sleep. If you’ve ever wondered why you wake up tired or whether you might have conditions like sleep apnea, this guide will help you navigate the technical procedures of conducting a sleep study. Understanding what’s involved can alleviate anxiety and empower you to take control of your sleep health. By the end, you’ll feel more prepared to discuss your concerns with a healthcare provider and explore your options for better rest. Let’s dive into the essentials of performing a sleep study and discover how it can be a crucial step toward restorative sleep and improved overall well-being.
How Sleep Studies Work: A Comprehensive Guide
Polysomnography, commonly known as a sleep study, is a comprehensive evaluation of sleep conducted to diagnose various sleep disorders. During a polysomnographic study, multiple parameters of sleep are recorded, providing a detailed snapshot of an individual’s sleep patterns. This test typically takes place overnight in a sleep lab where patients are monitored closely. Essential to the process are electrodes and sensors that track brain waves, muscle activity, heart rate, oxygen levels, and breathing patterns, allowing sleep technicians to analyze the data for irregularities or disturbances.
The technical procedure of a sleep study involves several critical steps. First, the patient arrives at the sleep clinic, usually in the evening, where a sleep technician prepares them for the study. After being shown to their private room, small electrodes are placed on the scalp, face, chest, and legs to monitor brain activity, eye movements, and muscle tone. Elastic belts may be placed around the chest and abdomen to measure breathing effort, while a pulse oximeter monitors oxygen levels. Once equipped, the patient lies down in a comfortable bed, and the study begins as they transition into sleep. A computerized system records all the collected data overnight.
In the event of disturbances such as sleep apnea, the testing equipment can note interruptions in breathing, oxygen saturation drops, and variations in heart rate, helping clinicians to make informed diagnoses. The results of the sleep study are then analyzed after the fact, often requiring thorough interpretation by a sleep specialist who considers the collected data alongside the patient’s symptoms and medical history.
Understanding how sleep studies work not only demystifies the process but also empowers individuals suffering from sleep issues to seek necessary help earnestly. If you’re experiencing ongoing sleep difficulties, a polysomnography may be an essential tool for improving your sleep health.
The Different Types of Sleep Studies Explained
Polysomnography, commonly referred to as a sleep study, comes in various forms, each tailored to assess specific sleep-related issues. Understanding these different types can help you navigate your options and make informed decisions about your sleep health.
Types of Sleep Studies
The most comprehensive type is the Polysomnography (PSG), which is performed in a sleep lab. This overnight study captures a wide array of data, including brain waves, oxygen levels, heart rate, and breathing patterns. It is the gold standard for diagnosing many disorders, such as sleep apnea, insomnia, and narcolepsy. It typically involves the placement of multiple sensors and electrodes on the body, allowing for detailed monitoring throughout the night.
Another common type is the Home Sleep Apnea Test (HSAT). This option is convenient for individuals suspected of having sleep apnea and can often be done in the comfort of your home. A simplified device is used that typically measures oxygen levels and airflow, alongside heart rate and respiratory effort. While this test does not capture all the data that a PSG would, it can still provide valuable insights, especially for those who may have concerns about the sleep lab environment.
Additionally, there are Multiple Sleep Latency Tests (MSLT) and Maintenance of Wakefulness Tests (MWT). Both of these tests are generally conducted during the day to assess sleepiness levels. The MSLT measures how quickly you fall asleep during a series of naps, thereby evaluating your tendency to sleep. The MWT, on the other hand, tests the ability to stay awake in a quiet, dimly lit environment. These tests are particularly useful for identifying conditions like narcolepsy or excessive daytime sleepiness.
Lastly, Actigraphy is another method where a wrist-worn monitor tracks movement to infer sleep patterns over a longer period (typically a week). This non-invasive approach can help identify sleep quality and quantity, making it a good option for those who might not need an in-depth sleep study.
Choosing the right type of sleep study depends on your specific symptoms and the recommendations of your healthcare provider. Remember, it’s important to discuss your concerns thoroughly, which can help in selecting the most appropriate testing method for your situation.
What to Expect During Your Sleep Study
A sleep study can be a significant step toward uncovering potential sleep disorders, but it’s normal to feel a bit anxious about what to expect. Rest assured, understanding the process can help ease your fears. During a typical polysomnography (PSG), various monitors will record essential data that offers insights into your sleep patterns. This often includes measurements of brain waves, oxygen levels, heart rate, and respiratory patterns, all crucial for diagnosing conditions like sleep apnea or insomnia.
When you arrive at the sleep lab, you will typically be welcomed by a sleep technician who will explain the procedure and help you get settled. Expect a comfortable environment; your sleeping area may resemble a hotel room, complete with a bed and soft lighting. As part of the setup, the technician will attach small electrodes to your scalp and face, along with sensors on your chest and legs. This may sound intimidating, but the electrodes are painless and do not disrupt sleep significantly.
Here are a few things you can prepare for to make your sleep study experience smoother:
- Bring comfortable pajamas: This can enhance your ability to relax and fall asleep.
- Avoid caffeine and stimulants: Limit these, especially on the day of your study, to ensure better sleep quality.
- Discuss any medications: Make sure your sleep technician knows about any medications you are taking, as this can impact the study.
As the night progresses, you should feel at ease-your monitoring equipment is designed to be unobtrusive. The technician will be monitoring you from another room, ensuring they can assist if needed without interrupting your sleep. In the morning, the study will end, and you will disconnect from the sensors. Although it may feel strange at first, many find they can sleep well despite the equipment.
Finally, remember that a sleep study is a critical tool in your journey toward better sleep health. It can provide your healthcare provider with the detailed information needed to tailor an effective treatment plan. Taking this step can pave the way for potentially life-changing insights into your sleep quality, allowing you to address problems and improve your overall health.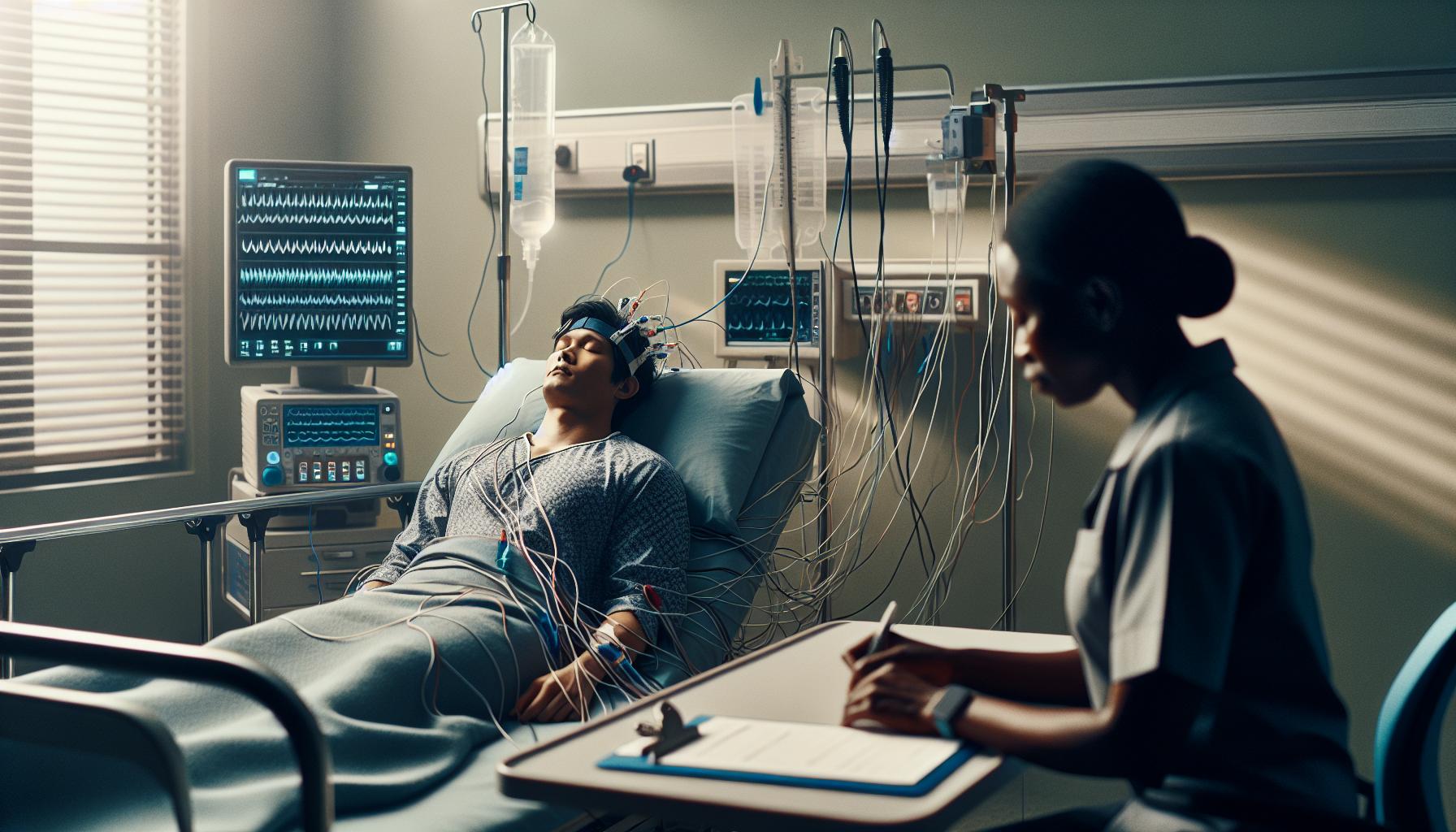
Preparing for Your Sleep Study: Essential Steps
Understanding how to effectively prepare for a sleep study is essential for maximizing the benefits of this important diagnostic tool. Getting a good night’s sleep during your study is not just about comfort; it also plays a critical role in the accuracy of the results. Preparation can help ease any anxiety and ensure that you are ready for the experience ahead.
Before your sleep study, it’s important to follow specific guidelines that can influence the quality of your sleep and the data collected. Start by avoiding alcohol and caffeine in the afternoon and evening before your test. Both substances can significantly disrupt your sleep patterns, which may lead to inaccurate results. Additionally, if you are taking medication that affects sleep, make sure to discuss it with your healthcare provider beforehand; they may suggest adjusting your dosage or timing, as some medications can interfere with the study results.
Packing for your sleep study also contributes to a smoother experience. Bring comfortable pajamas that allow you to move freely, as well as any personal items that help you relax, such as a favorite pillow or blanket. It’s also wise to prepare your mind for sleep-consider techniques like deep breathing or light reading to help ease you into a restful state during your study.
On the day of your test, aim to arrive at the sleep center with plenty of time to spare. This allows you to familiarize yourself with the environment and ask any last-minute questions. Remember that the sleep technician is there to help-don’t hesitate to voice your concerns or inquire about the monitoring process. You’ll find that understanding what to expect can significantly reduce anxiety, paving the way for a successful sleep study outcome.
Understanding Polysomnography and Its Importance
Polysomnography, commonly known as a sleep study, is a comprehensive assessment that plays a crucial role in diagnosing a wide array of sleep disorders. This elaborate procedure allows healthcare professionals to gather detailed physiological data during various stages of sleep, providing insight that is vital for effective treatment. Understanding how polysomnography works and its significance can empower individuals to make informed decisions about their sleep health.
During a polysomnography, several physiological parameters are monitored, including brain activity (via electroencephalogram or EEG), heart rate, breathing patterns, and blood oxygen levels. This multipronged approach enables clinicians to observe a patient’s sleep architecture, comprising different sleep stages such as REM and non-REM sleep. By analyzing this data, healthcare providers can identify specific disorders like sleep apnea, restless leg syndrome, and narcolepsy. For instance, the ability to monitor breathing can reveal intermittent obstruction, a hallmark of sleep apnea, which if left untreated, can lead to serious health issues such as cardiovascular problems and daytime fatigue.
The importance of polysomnography extends beyond mere diagnosis. It serves as the foundation for tailored treatment options that can significantly improve quality of life. For example, understanding a patient’s unique sleep profile can guide treatment plans ranging from lifestyle modifications and continuous positive airway pressure (CPAP) therapy for sleep apnea, to cognitive behavioral therapy for insomnia. Moreover, recognizing the implications of sleep patterns can motivate individuals to prioritize sleep health, ultimately fostering a healthier lifestyle.
Polysomnography is typically conducted in a sleep center, where advanced technology and professional oversight create a controlled environment. While some individuals may feel apprehensive about undergoing a sleep study due to the unfamiliar setting or equipment, knowing that it is a safe and non-invasive process can alleviate anxiety. Technicians are skilled in creating a supportive atmosphere, ensuring patients feel comfortable and informed throughout the study. Understanding the procedure, including what data is collected and how it is utilized, can empower individuals to approach their sleep health with greater confidence and proactive engagement.
Common Sleep Disorders Detected in Studies
Many people struggle with sleep-related issues, often unaware that they could be suffering from a sleep disorder. Polysomnography, commonly referred to as a sleep study, is a powerful diagnostic tool that helps identify various conditions that disrupt sleep. Understanding the most common disorders detected in these studies can empower you to make informed decisions about your sleep health.
- Sleep Apnea: Perhaps the most well-known disorder, sleep apnea is characterized by repeated interruptions in breathing during sleep. This condition often leads to snoring and can result in fragmented sleep and daytime fatigue. Polysomnography allows for the monitoring of breathing patterns and oxygen levels, indicating whether a person experiences apneas (pauses in breathing).
- Insomnia: Insomnia manifests as difficulty falling asleep or staying asleep. Sleep studies can help differentiate between primary insomnia and insomnia secondary to other conditions, offering insights into a patient’s sleep architecture and the factors affecting their sleep quality.
- Restless Leg Syndrome (RLS): Individuals with RLS experience an uncontrollable urge to move their legs, often accompanied by uncomfortable sensations. This can severely disrupt sleep. Polysomnography can capture these movements during sleep, facilitating a diagnosis.
- Periodic Limb Movement Disorder (PLMD): This condition involves involuntary leg movements during sleep, which can lead to awakenings and reduced sleep quality. A sleep study can observe the frequency and nature of these limb movements, aiding in diagnosis.
- Narcolepsy: This neurological disorder affects the brain’s ability to regulate sleep-wake cycles, leading to excessive daytime sleepiness and sudden sleep attacks. The study can monitor sleep onset and the presence of REM sleep at inappropriate times, which is key for diagnosing narcolepsy.
Understanding these common disorders is crucial for anyone experiencing sleeping issues. Polysomnography not only facilitates the diagnosis of these conditions but also serves as a basis for creating tailored treatment plans. If you suspect you might be affected by any of these sleep disorders, consider discussing a sleep study with your healthcare provider. Taking this proactive step can lead to improved sleep quality and, ultimately, better overall health.
The Role of Wearable Sleep Trackers
Wearable sleep trackers have surged in popularity as more people become aware of their sleep health. These devices, ranging from smartwatches to specialized rings, promise insights into sleep patterns, duration, and even the quality of sleep, delivering data that can empower individuals to make better lifestyle choices. However, it’s important to weigh their convenience and accessibility against their accuracy and reliability when it comes to understanding your sleep.
Being non-invasive and user-friendly, wearables typically track metrics such as heart rate, movement, and even light exposure, providing a portrayal of sleep stages. Most devices will categorize your time in light, deep, and REM sleep, which can be particularly engaging for those seeking to enhance their overall wellness. However, despite their appeal, the accuracy of these devices can be inconsistent. For instance, a study found that wearables often do not align perfectly with the results of traditional polysomnography, which is considered the gold standard in sleep diagnostics [[2]]. This discrepancy raises questions about how much reliance should be placed on their results.
It’s also essential to consider the psychological impact of using these trackers. While the data can be helpful, some users report anxiety over their sleep scores, which can ironically lead to poorer sleep quality. If tracking your sleep adds to your stress, it may be worthwhile to take a break from these devices to focus on calming your mind-after all, quality sleep is often about the relaxation you can achieve, not just the data you gather [[1]].
In summary, while wearable sleep trackers offer a convenient and engaging way to monitor sleep, users should approach them with a critical mind. They can serve as a useful initial tool, but for more serious sleep concerns, consulting a healthcare provider is a prudent step. Understanding the limitations and the technology behind these wearables can help individuals make informed choices about managing their sleep health.
Home Sleep Tests vs. In-Lab Sleep Studies
Home Sleep Tests and In-Lab Sleep Studies offer distinct approaches to diagnosing sleep disorders, each suited for different scenarios and patient needs. Understanding these differences can empower you to make informed choices about your sleep health.
In-lab sleep studies, or polysomnography, are conducted in a specially designed sleep clinic or lab. You can expect a comprehensive evaluation that records various biological signals such as brain waves, heart rate, breathing, and eye movements throughout the night. This controlled environment allows for precise monitoring by trained professionals, providing a detailed analysis of your sleep stages, including light, deep, and REM sleep. While this option is considered the gold standard for diagnosing conditions like sleep apnea or narcolepsy, it often involves higher costs, greater time commitment, and potential discomfort due to the number of sensors attached to the body.
On the other hand, home sleep tests (HST) offer a more convenient and cost-effective alternative. These tests come as portable devices that you can use in your own bed, and they primarily focus on monitoring parameters like oxygen levels and airflow – key indicators of sleep apnea. Home tests have gained popularity due to their simplicity and the comfort of sleeping in familiar surroundings. However, they may not provide as comprehensive data as in-lab studies and are primarily effective in diagnosing obstructive sleep apnea, leaving other sleep disorders undetected.
When considering which option to pursue, think about your specific symptoms, lifestyle, and health insurance coverage. In-lab studies may be necessary for complex cases or to rule out multiple disorders, while HSTs can serve well for straightforward apnea assessments. Whichever route you choose, consult with your healthcare provider to find the best fit for your needs and circumstances.
Insurance Coverage for Sleep Studies: What You Need to Know
Navigating the insurance coverage for sleep studies can feel overwhelming, but understanding your options is crucial for maximizing your benefits and minimizing out-of-pocket costs. Many health insurance plans do cover sleep studies as they are recognized as necessary diagnostic tools for various sleep disorders, including sleep apnea, insomnia, and narcolepsy. However, coverage can vary significantly from one policy to another. It is pivotal to check with your specific insurance provider to determine what is included in your plan.
When it comes to costs, in-lab sleep studies tend to be more expensive than home sleep tests, primarily due to the comprehensive nature of the testing and the involved personnel. For instance, an in-lab study can range from $1,000 to $3,000 or more, whereas home tests might be covered under different conditions or at a much lower cost. Many insurance policies do require pre-authorization for these procedures, especially if you are seeking an in-lab study for complex symptoms. You may need to provide documentation of previous attempts to address your sleep issues through less invasive means.
It’s also worth noting that some insurance plans have specific criteria regarding which patients can qualify for sleep studies. Generally, factors such as age, weight, and documented symptoms will influence the approval process. For example, many insurers are more likely to approve an in-lab sleep study for patients with notable risk factors for sleep apnea, such as obesity or a history of sleep-related breathing disorders, compared to those without these indicators [1[1].
Always ask your healthcare provider or sleep specialist about the most appropriate study for your needs and get assistance navigating your insurance options. You can also look into flexible spending accounts (FSAs) or health savings accounts (HSAs) that may help you manage unexpected costs associated with your sleep study. By being informed and proactive, you will be better equipped to make decisions that enhance your sleep health without undue financial stress.
Decoding Your Sleep Study Results: Key Insights
Understanding your sleep study results can be both enlightening and daunting. It’s crucial to approach the data with a clear mind and a bit of guidance. Sleep studies primarily evaluate your sleep patterns, breathing, and overall sleep quality, allowing practitioners to diagnose potential issues such as sleep apnea, insomnia, or other sleep disorders. The results are typically presented in a structured report that breaks down various metrics.
A key component of your sleep study report is polysomnography data, which reflects different sleep stages: light sleep, deep sleep, and REM sleep. Each stage has distinct characteristics and functions, impacting how rested you feel. For example, insufficient deep sleep can lead to daytime fatigue and cognitive issues. If your report indicates that you’re not spending enough time in these restorative stages, it may signal an underlying condition that needs to be addressed.
In addition, the report usually includes details on your breathing patterns throughout the night. If you notice mentions of apneas-instances where your breathing stops for brief periods-it could point to obstructive sleep apnea (OSA). This condition can lead to serious health issues if left unchecked. Your healthcare provider will explain how many apneas occurred, their duration, and how they corresponded to sleep stages, giving you a clearer picture of your sleep health.
To decode your results effectively, consult with your sleep specialist. They can provide personalized insights and recommendations based on your data. Don’t hesitate to ask questions about anything that feels unclear, such as device accuracy or the implications of your findings. Taking your time to understand your sleep study can empower you to make informed decisions about your health, potentially leading to better sleep and improved quality of life.
Troubleshooting Common Issues with Sleep Studies
Common concerns arise when preparing for or undergoing a sleep study. Understanding and addressing these issues can significantly enhance your experience and ensure accurate results. Many participants worry about the comfort of the testing environment or the potential disruption to their sleep patterns due to the equipment used. Here’s how to troubleshoot those common challenges.
To start, if you anticipate difficulties falling asleep in an unfamiliar environment, consider talking to your doctor about your options for pre-study sleep aids. Some individuals find that light sedation can help ease anxiety and facilitate a restful night. It’s crucial to communicate any concerns about sleep medications with your healthcare provider, as they can provide guidance on manageable choices that align with your sleep study’s objectives.
Equipment Comfort and Setup
Many participants express discomfort with the various sensors and wires necessary for monitoring sleep. A proactive approach is to familiarize yourself with the setup process beforehand. Here are a few tips for a smoother experience:
- Test the equipment: Before the night of the study, practice wearing similar equipment if available. This helps reduce anxiety about the unknown.
- Ask for assistance: Don’t hesitate to ask the sleep technician for help during setup. They can provide tips on how to comfortably position yourself with all the cables and monitor connections.
- Bring familiar items: Consider bringing personal items, such as a pillow or blanket, to create a more comforting atmosphere that mirrors your sleeping environment at home.
Sleep Disruptions
Unexpected awakenings during the study can occur, and it’s essential to remember that these are typically part of the process. Sleep studies often involve periodic awakenings to assess different stages of sleep. If you find that you are awakened more often than anticipated, try to stay calm and focus on returning to sleep rather than stressing about the disruptions.
For some, difficulty sleeping through the night can lead to an incomplete sleep study, which can impact diagnostic accuracy. If you’re struggling, let the staff know; they might suggest adjustments or provide techniques for relaxation that can help enhance your overall sleep quality during the study.
Overcoming these common issues with preparation and proactive communication can transform your experience from daunting to manageable. Sleep studies provide vital insights into your sleep health, and addressing challenges effectively ensures a more productive assessment of your sleep pattern and quality.
When to Seek a Sleep Study vs. Using Sleep Trackers
Recognizing when to seek a sleep study versus relying on sleep trackers can be pivotal in addressing your sleep issues effectively. Sleep studies, particularly polysomnography, are comprehensive tests that measure various bodily functions during sleep, including brain waves, oxygen levels, heart rate, and breathing patterns. If you experience symptoms such as excessive daytime sleepiness, loud snoring, gasping for air during sleep, or persistent insomnia, a sleep study is essential for an accurate diagnosis of potential sleep disorders like sleep apnea or restless leg syndrome.
On the other hand, sleep trackers offer insights into your sleep patterns and behaviors but should be considered more of an initial step rather than a definitive solution. These devices can help you monitor sleep duration and quality, potentially helping identify issues like inconsistent sleep routines. However, they do not replace professional evaluations, as they lack the capability to diagnose medical conditions and can sometimes deliver misleading information due to differences in algorithm accuracy between devices [[1](https://www.hopkinsmedicine.org/health/wellness-and-prevention/do-sleep-trackers-really-work)][[3](https://www.bannerhealth.com/healthcareblog/advise-me/are-wearables-reliable-for-tracking-sleep-what-you-need-to-know)].
### When to Choose Which Option
Situations Favoring Sleep Studies
- Persistent Symptoms: If you have chronic fatigue, loud snoring, or witness breathing interruptions.
- Risk Factors: A family history of sleep disorders, obesity, or other health issues that complicate sleep.
- Seeking Medical Advice: If your initial assessments through trackers suggest concerning trends that warrant further investigation.
Cases for Sleep Trackers
- Casual Monitoring: Use trackers to get a general sense of your sleep patterns and habits.
- Early Stage Investigation: When you want to identify trends in your sleep without immediate medical concerns.
- Personal Insights: Trackers can help you adjust behaviors like bedtime routines or caffeine intake.
Ultimately, the decision between a sleep study and a sleep tracker depends on the severity and frequency of your symptoms. If in doubt, discuss your concerns with a healthcare provider who can guide you based on your specific circumstances and health history.
Faq
Q: What is the purpose of a sleep study?
A: A sleep study, or polysomnography, evaluates sleep patterns to diagnose disorders like sleep apnea, insomnia, and narcolepsy. It records brain activity, breathing, and other vital functions while you sleep, helping identify issues affecting sleep quality and overall health.
Q: How long does a sleep study typically take?
A: A standard sleep study lasts about 7 to 8 hours, as it aims to capture a full night of sleep. Some tests, like daytime naps or home sleep tests, may take less time. Always check with your provider for specific timelines related to your study.
Q: Do I need special preparation for a sleep study?
A: Yes, preparation is essential! Avoid caffeine and alcohol on the day of the study, and follow any specific guidelines provided by your healthcare provider, like bringing pajamas or avoiding certain medications. For detailed steps, refer to our section on “Preparing for Your Sleep Study.”
Q: What equipment is used during a sleep study?
A: During a sleep study, you may wear sensors for monitoring brain waves, heart rate, breathing, and blood oxygen levels. These devices help medical professionals analyze your sleep stages and detect any abnormalities.
Q: Can I sleep normally during a sleep study?
A: Yes, the goal is to allow you to sleep as normally as possible. Technicians will monitor you closely, ensuring minimal disturbances while capturing your natural sleep patterns. Your comfort is a priority to achieve accurate results.
Q: Are home sleep tests effective compared to in-lab studies?
A: Home sleep tests can be effective for diagnosing conditions like obstructive sleep apnea but may not capture the full range of sleep disorders as in-lab studies do. Consult your doctor to determine which option best suits your symptoms and medical history.
Q: How are sleep study results provided to me?
A: After your sleep study, a specialist will analyze the data and prepare a report. Your healthcare provider will discuss the results with you, explaining any findings and recommending treatment options based on your specific condition.
Q: What should I do if I feel anxious about a sleep study?
A: It’s normal to feel anxious about a sleep study. Talk to your healthcare provider about your concerns; they can provide reassurance and details on what to expect, which can help alleviate anxiety. Understanding the process often eases worries.
To Wrap It Up
Ready to take control of your sleep health? A sleep study may be the next crucial step if you suspect sleep disorders like sleep apnea or chronic insomnia. By understanding the procedure, from setup to monitoring, you can approach your sleep study with confidence. Remember, the insights gained can lead to better sleep solutions tailored just for you.
For more details on what to expect, explore our comprehensive guides on sleep disorders and device comparisons to choose the right wearable for your needs. Don’t forget to check out our helpful tips on preparing for a sleep study and insurance navigation.
Stay informed and proactive about your sleep health-sign up for our newsletter for the latest updates and expert insights. Share your thoughts or questions in the comments below, and let’s embark on this journey to restful nights together!